Questions Parents Often Ask About a Birth: “Why wasn’t my baby breathing when born?” . . . “Why did my baby’s skin look blue?” . . . “What does a low or poor Apgar score mean?” . . . “What is causing my baby’s seizures?”
When a baby is delivered, each person in the room (including the health care professionals) are waiting with bated breath to hear the first cry and catch a glimpse of the pink tiny human. Sometimes, however, a newborn baby does not cry right away, or is a pale/bluish color after delivery. When this happens, the baby is often rushed to NICU. This can be quite frightening for parents. Below we answer questions parents often ask after a difficult birth and provide next steps to determining if a baby born with problems has lasting damages.
Why wasn’t my baby breathing when born?
There are several complications that can result in a baby born in respiratory distress. Between 2 and 10 out of every 1,000 newborns experience lack of oxygen. The most common reasons a baby is born not breathing include:
Why did my baby’s skin look blue?
When a child is born blue, there is always a flurry of activity in the delivery room. The reason a baby is born blue in color is because of poorly oxygenated blood. Blood pumps from the heart to the lungs, where it receives oxygen, then is circulated back through the heart and throughout the body. The condition of having blue-tinted skin is called cyanosis. Cyanosis is not always an emergency. Babies transitioning to life outside the womb may at first struggle to get oxygen, but it often resolves within a minute. If, however, your baby’s skin remained blue for longer than a minute, or had other symptoms at birth, it could be a sign of serious health problems.
What is causing my baby’s seizures?
The most common cause of neonatal seizures is hypoxic-ischemic-encephalopathy (HIE), a type of brain injury caused by a lack of oxygen during labor and delivery. HIE is a brain disfunction caused by a reduction in the supply of oxygen to the brain and other organs (hypoxia), compounded with low blood flow to vital organs (ischemia). Encephalopathy refers to any condition that results from reduced blood flow and oxygen supply to the brain. When oxygen deprivation occurs, there is a series of events that cause a decrease in energy production in the brain. This can cause the brain to produce a chemical that causes excessive excitation in a part of the brain called the cortex, resulting in seizures.
What are APGAR scores and what does a low APGAR score mean?
Apgar score is a test given one minute after a baby is born, and five minutes later. Sometimes, if there are concerns about the baby’s condition or the score at five minutes is low, the test may be scored for a third time at ten minutes after birth.
Five factors are used to evaluate the baby’s condition and each factor is scored on a scale of 0 to 2, with 2 being the best score:
A: Appearance (skin color)
P: Pulse
G: Grimace (reflex)
A: Activity (muscle tone)
R: Respiration
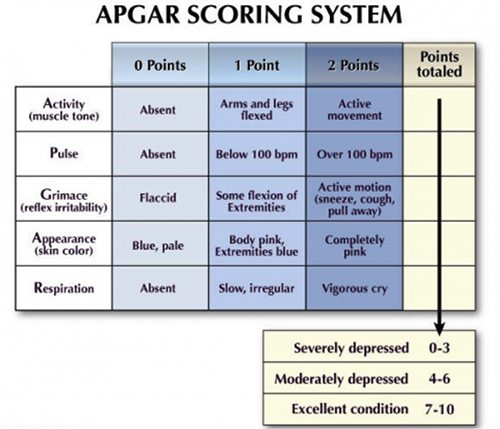
A perfect Apgar score is 10. A score lower than seven means that the baby might need help breathing. A low Apgar score does not mean a child will have serious or long-term health problems, as it is not meant to predict the future health of the child. For others, however, it may signal a serious and potentially life-threatening problem requiring immediate medical attention.
What should I do if I suspect negligence caused my baby’s injury?
Perhaps your newborn was sent to NICU right after birth. If you or someone close to you recently suffered a difficult labor or delivery and injury to the newborn that resulted in a stay in NICU, act quickly to preserve evidence. The only way to determine if the injury was avoidable is to have prenatal, delivery, and newborn medical care attentively reviewed by qualified professionals who understand the complex physiology of mother and fetus during gestation, stresses the baby undergoes during the birth, mechanisms to cope with the stresses, adjusting the newborn to life outside of the womb, and requirements and responses to stresses and factors in the environment.
At Buchanan Firm, our combined legal-medical team has decades of experience handling medical malpractice cases, especially birth injury and birth trauma. We have experienced medical professionals on staff to talk with you right away and review your claim. We quickly and efficiently to assess the medical facts and take immediate action to protect your rights. And, if we find malpractice caused injury, we will take the wrongdoer to court to secure fair and just compensation for the injured child.